How Dead is Dead Enough?
By Michael G. Darwin
April 30, 2008
Introduction
In 2002, two medications were eliminated from the stabilization protocol applied to cryopatients in order to provide protection against ischemia-reperfusion injury, post mortem clotting, the return of consciousness and spontaneous heartbeat, movement, or other evidence of life which might occur when blood circulation and breathing are artificially restored during cardiopulmonary support (CPS) and cooling after medico-legal death is pronounced death (1). These medications were the neuromuscular blocking paralytic vecuronium bromide (trade name Norcuron, a neuromuscular blocking (NMB) agent that paralyzes voluntary muscles) and potassium chloride (supraphysiologic concentrations of the potassium ion inhibit brain electrical activity (EEG) and both mechanical and electrical cardiac activity (ECG). These changes were made per the recommendation of Alcor Life Extension Foundation, Inc., (Alcor) and Suspended Animation, Inc., (SA) Medical Director Steven B. Harris, M.D. (2). The rationale for this change was that “These two drugs are associated with illegal acts of euthanasia and could cause serious legal complications if used on cryonics patients. These drugs were removed from use so that no one could claim that we ever used anything to hasten a patient’s death. The object was to insure that everything in the kit would be non-lethal. So, if there was a mistake and the cocktail was given too early and someone later claimed the patient was not formally (legally) dead we would have the back-up argument that nothing fatal was given anyway.” (2). A few staff members from several cryonics organizations have expressed the erroneous opinion that this change was made because these medications were “scheduled” or restricted in their distribution and possession by the United States (U.S.) Drug Enforcement Agency (DEA) pursuant to Federal law (5), (6). This was not the case.
This change in the cryopatient stabilization protocol (i.e., current cryonics corporate policy) has been (and continues to be) validated by a position recently very well articulated by a veteran cryonics professional when he stated: “I don’t think the issue is so much as to whether or not a given medication is scheduled, but whether it could be used to hasten death. If there is a legal entanglement, officials might question if the medication in question could have been used pre-mortem. If we don’t have anything like that in the kits it makes it easier to defend our position…As long as our meds protocol does not point fingers in our direction we can feel reasonably secure. I’ve heard management tell members of the press as well as the general public numerous times there is nothing in our kits that can be used to hasten death. (9).”
This is now the dominant view within the cryonics community. I believe this position is incorrect and that it provides a dangerous sense of false security, and further, that it obscures discussion and action on deeper issues that will have to be addressed, either sooner, in a calm, prospective manner, or later, in the midst of crisis, strong emotions and retrospective blaming.
All Drugs Are Poisons
Every medical student and all forensic medical personnel are taught that “all drugs are poisons” in pharmacology 101. This is not an empty cliché, but rather an important fact that ultimately underpins and guides the most basic practice of medicine. This realization is one of the primary reasons why good physicians are reluctant to prescribe more than the absolute minimum of medications to their patients, and why they often leave non-life threatening conditions un-medicated despite the inconvenience and discomfort this may cause. While this dictum may become less true as pharmacology becomes more sophisticated, and medications become more targeted and specific, today, it is as true as it ever was.
The idea that the current Alcor or SA medication protocol is benign or somehow consists of drugs which do not evoke concerns over euthanasia, or hastening of cryopatients’ deaths, is mistaken. Propofol ( Diprivan™), given as the first medication, and used to reduce cerebral metabolism and prevent return of consciousness during CPS (10) is a sedative-hypnotic-anesthetic which has been responsible for many patient deaths worldwide in both the operative procedures and in ICU† (11) . There is currently intense and often vituperative debate between anesthesiologists, intensivists and other physicians about whether this drug should be administered by anyone other than anesthesiologists or nurse anesthetists; especially in outpatient settings or to critically ill or hemodynamically unstable patients (12), (13), (14). Even more to the point, because veterinary barbiturate-based euthanasia products result in a high incidence of undesirable side effects, such as tonic-clonic spasms, gasping, yawning or muscle vesiculations (15), it is good practice (indeed the standard of care) that animals be pre-medicated with a sedative or tranquilizing agent such as tiletamine/zolazepam or xylazine (16). Furthermore, for the aforementioned reasons and because all barbiturate-based veterinary euthanasia products are controlled substances, Schering-Plough (a leading manufacturer of veterinary drugs) is in development of a propofol-based euthanasia formulation that would combine propofol and phenytoin in much the same way as barbiturate and phenytoin are combined in standard veterinary euthanasia products such as Euthanol™(see US Patent 5,962,536; the inventor, Gene Kormer, is an employee of Schering-Plough in Fort Collins, CO) (17). If this product is introduced into the marketplace it will reposition propofol as a euthanasia agent as well as a sedative-hypnotic used to alleviate pain and agitation and induce anesthesia in veterinary and human medicine (18), (19).
Having used propofol extensively in animal research, I believe that it is highly likely (indeed all but a documented a certainty) that propofol has already been used in clinical medicine to affect euthanasia. The drug is very rapid acting and when given too quickly, or at too high a dose, can induce hypotension and cardiovascular collapse (18), (20). It’s ready availability, widespread use in critically and terminally ill patients, and above all its lack of scheduled status, unarguably make it one of the most conveniently available agents (alone or in combination with other drugs such as lidocaine, phenytoin (Dilantin™) potassium chloride, etc.) for ad hoc consensual euthanasia – or for serial murder by the all too common sociopathic/homicidal physician or nurse who acts out in a medical setting (21), (22). I believe that it is only a matter of time before propofol is publicly implicated in a case of euthanasia (consensual or otherwise) brought to criminal prosecution. While it can be fairly argued that this is solely a matter of opinion on my part, I submit that it is an opinion strongly grounded in a commonsense and an obvious application of the drug given its pharmacology, ubiquitous use, and lack of controlled status. It is also not necessary to rely on my opinion alone; the opinion of professionals in critical care medicine and end-of-life issues should be solicited on this matter.
Some Currently Used Stabilization Medications Are Potentially Lethal
Beyond propofol, there are both the general and specific issues of using compounds that are completely outside of conventional medical and forensic experience (10). This, perhaps more than any other practice, is likely to arouse both medical and legal forensic curiosity and concern. One of the unfortunate changes in cryonics over the past decade has been the relative isolation of cryonics caregivers from the research environment. Because the number of cryopatients treated is so low, and because these patients are already in cardiovascular collapse and are not monitored for the effects of stabilization drugs on hemodynamics, stabilization personnel lack both visceral and intellectual understanding of the powerful adverse effects of novel molecules such as kynurenine, 4-hydroxy-tempol (TEMPOL), or, for that matter, the vehicle solution used to deliver melatonin, PBN and vitamin E in the proprietary antioxidant cocktail VitalOxy™ marked by Critical Care Research, Inc., (CCR) of Rancho Cucamonga, CA.
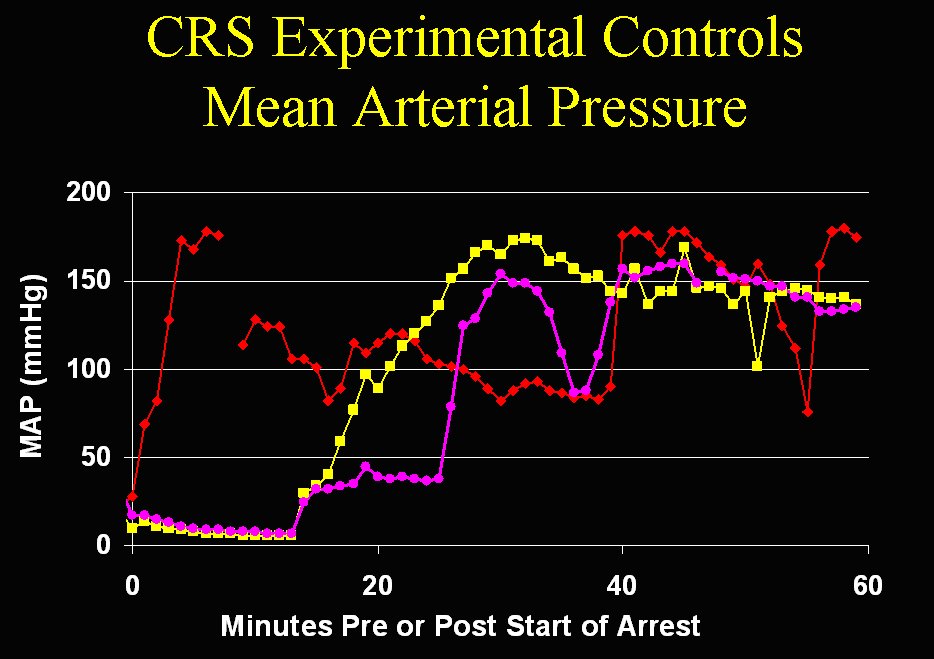
In the course of 4 years of animal research using this combination of drugs (and emulsifying vehicle) in the 21st Century Medicine, Inc. (21CM) Canine Resuscitation Series (CRS) experiments (which now serves as the basis for both Alcor’s and SA’s stabilization medications protocol), my colleagues and I at 21CM (and later CCR) became very familiar with their adverse hemodynamic effects and potential to cause cardiovascular collapse and death. Indeed, these effects were a constant obstacle to their therapeutic application which required aggressive intervention with pressors and careful titration of the rate of administration. Kynurenine results in a dramatic reduction of mean arterial pressure (MAP) even in the presence of the highly potent pressors vasopressin and epinephrine, both of which were given in substantially supra-clinical doses in the CRS experiments (23). This is borne out by the data from these experiments as shown below in Figures 1 and 2. The control animals (not given active drugs or vehicles) had the expected profound hypertensive response to pressors given at the start of reperfusion.
Figure 1: Hypertensive hemodynamic response exhibited by control dogs in response to multiple doses of epinephrine and vasopressin followed by continuous infusion of dopamine and s-methyl-isothiourea (SMT) during cardiopulmonary bypass-initiated and assisted reperfusion following 15 to 16 minutes of normothermic whole body ischemia. (Courtesy of Critical Care Research, Rancho Cucamonga, CA)
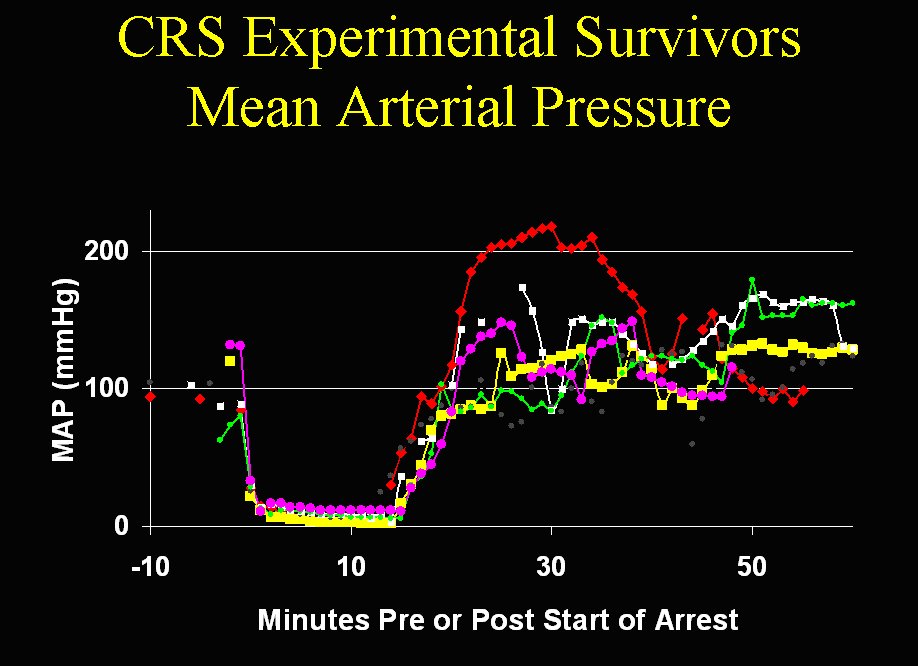
By contrast, the experimental group experienced marked depression of MAP even with repeated dosing of vasopressin and epinephrine (not shown in the graph) and continuous administration of both dopamine (a potent beta adrenergic agonist) and SMT (which facilitates an increase in MAP due to its eNOS inhibiting properties) as seen in Figure 2, below.
Figure 2: Blunted hypertensive response exhibited by experimental dogs receiving hypotension-inducing cerebroprotective drugs in response to multiple doses of epinephrine and vasopressin followed by continuous infusion of dopamine and s-methyl-isothiourea (SMT) during cardiopulmonary bypass-initiated and assisted reperfusion following 15 to 16 minutes of normothermic whole body ischemia. (Courtesy of Critical Care Research, Rancho Cucamonga, CA)
Similarly, the marked hypotensive effect of TEMPOL has been documented in the literature as shown in Figure 3 below and there is evidence that many potent free radical scavengers may induce hypotension (24).
Figure 3 (left) : Dose-dependant effect of the free radical spin trap 4-hydroxy-TEMPOL on mean arterial pressure in the rat (24).
The Dull Gray Line
I believe it is unwise to presume that just because these drugs have no history of use in homicide or active euthanasia that the conclusion can be drawn that they will be viewed as forensically benign. In fact, it is not the use of any given drug in cryonics stabilizations, per se, that may arouse suspicion or cause legal complications, but rather the milieu in which any drugs are administered. More precisely, exposure to risk depends upon the degree of clarity and brilliance of what I call the “dull gray line” between the end of medical care and life (i.e., pronouncement and the presence of perceived irreversible cessation of vital functions) and the start of any cryonics-related procedures. If referring to a dull gray line with words like “clarity” or “brilliance” seems oxymoronic, it is because it is; and therein in lies the danger.
The clarity and brilliance of the dull gray line increases steadily when the following conditions pertain:
a) There is absolutely no cryonics-related medical consultation/intervention in the patient’s medical care or management before or during his terminal illness. (This includes any consultation or input that might be suggested to the patient’s treating physician.)
b) The patient does not in any way self-medicate to minimize or eliminate ischemic injury that will result post-arrest.
c) The patient is surrounded and cared for by non-cryonicists who are indifferent or hostile to cryonics during his terminal illness.
d) The patient instructs (and follows through) that palliative medical management of pain and anxiety during his terminal illness be minimized (i.e., despite possible medical need that very high doses of opiates, benzodiazepines or other potentially lethal drugs associated with active euthanasia and violation of the rule of double effect not be used).
e) The first responder who removes the patient from the home is a mortician or body removal service whose sole cryonics related intervention is packing the patient in ice prior to, during, or after transportation to a mortuary or to cryonics organization facilities. Put another way: when the only cryonics intervention is modestly earlier implementation of an already accepted and widely practiced post mortem intervention; refrigeration to slow decomposition.
f) There is never any attempt to restore circulation, oxygenation, or to attempt to restore metabolism in any way. And conversely, that there is no attempt of any kind to inhibit or reduce metabolism other than by simple refrigeration as would be acceptable in the normal course of slowing or halting decomposition in a cadaver.
Darwin’s Laws of Conservative Cryonics
The above represents an envelope of relative safety in “caring” for cryopatients because one fundamental principle is adhered to: No actions are taken at any point in the relationship with the patient (from good health through transfer of custody to the cryonics organization) that deviate from those deemed acceptable and in accordance with extant medico-legal standards for the handling of a corpse until the time at which unequivocally lethal and irreversible actions, such as autopsy, embalming, interment or cremation are deemed medico-legally and socially acceptable. I call this Darwin’s First Law of Conservative Cryonics (the word “cowardly” may be substituted for “conservative, “as desired).
As soon as Darwin’s First Law is violated risk begins to attach to the care given the cryopatient. While it can (and should) be argued that some interventions will carry more risk than others, and that some drugs may provoke a more visceral or more aggressive response from medical and legal authorities, it cannot be argued that the risk is nonexistent or even small. One way of evaluating that risk is with Darwin’s Second Law of Conservative Cryonics which states that “the more temporally remote a cryonics intervention is from the time of certification of medico-legal death, the less likely it is to provoke adverse legal or forensic intervention.” Wait until putrefaction sets in, per the argument advanced by Jean-Jacques Winslow† that putrefaction is the only sure sign of death, and you will be as safe as it is possible to be.
Hopefully, no responsible cryonics organization will follow Darwin’s first two laws blindly, but rather, will use Darwin’s Third Law of Conservative Cryonics which posits that “forensic attacks on cryonics procedures are best defended against with forensic protections.” Forensic protections come in two forms. The first and most obvious is to establish policies and procedures which serve to insulate the cryonics care providers from both perceived and actual situations where their actions might violate the law. Some of these precautions, such as stabilization staff not being in the presence of actively dying patients absent disinterested medical staff or family, and the injunction against cryonics organization personnel providing any enabling advice or counsel regarding active euthanasia, have long been in place (25). However, arguably the most potent tools to guard against accusations of pharmacological foul play are the use of “as soon as possible” (ASAP) sampling and archiving of the patient’s blood post-pronouncement and prior to the administration of any stabilization drugs, as well as comprehensive videography of all stabilization procedures. Unfortunately, these procedures have been abandoned or even prohibited (26), (27). The advent of compact, reliable and wearable video recording equipment that could be deployed on the persons of stabilization Team members, as well as the ready and affordable availability of continuous, forensically certifiable, digital video recording equipment with the capability of uninterrupted recording of 2-weeks of ~250 to 450 frame per second
Figure 4: Cylon Body Worn Surveillance System. Wearable DVR: 16 x 9 screen size 720 x 576, resolution 4”, display video playback – MPEG-4 SP with stereo sound. Near DVD quality up to 720×480 @ 30 f/s (NTSC), 720×576 @ 25 f/s (PAL), AVI file format. WMV9 up to 352×288 @ 30 f/s, and 800 KBit/s. Exview Camera: Instant auto focus, Hi Resolution – 1 Lux 2 CIF image, rugged, waterproof, heat resistant and can be integrated into helmets and headwear. (Photos courtesy of The Audax Group, Plymouth, South Devon, UK, http://www.audaxuk.com/cylon/index.htm)
high quality color video (each terabyte of memory now costs approximately $400.00) have not been exploited by cryonics organizations‡. High capacity digital video recorders which allow for fast and easy data searches, provide self-schedule management, automatic data backup, e-mail event alert, and offer IP Address Dispatch (for use with dynamic IP), and control of multiple systems from a remote location (28) are now in wide use in law enforcement, government and business . In-house and in-field (mobile) versions of forensic video systems are rapidly becoming the standard of practice for law enforcement where they are used to protect police officers against accusations of abuse or misconduct (29), (30). One example widely used by law enforcement around the world is the Cylon Body Worn Surveillance System. The unit consists of a compact, waterproof DVR, and a high resolution color camera (worn on a headset) as shown in Figure 4, above. The DVR can store 400 hours of Mpeg-4 quality full color video and audio recording on it 100 GB hard drive and has a battery life of ~12-hours at its peak, 30 fps recording rate. Since the unit is built for law enforcement it has time/date stamping and event marking capability as well as sophisticated graphical user interface software which allows for rapid search and retrieval of recorded material (31).
It is more than a little bizarre and ironic that cryonics organizations, largely comprised of and operated by technophiles focused on the leading edge of information technology, have failed to adopt these advances, while governments, military and law enforcement agencies have rushed to embrace them in their earliest implementations.
Signs of Life, Irreversibility, and Medical Consensus on Pronouncing Death
The concerns over immediate (or as rapid as practical) application of post-arrest interventions† in the care of cryopatients fundamentally hinges on two issues:
a) Has the patient’s medico-legal death been hastened by the antemortem administration of any medication, and in particular any medication which is subsequently administered after pronouncement?
b) Will the patient experience auto-resuscitation as a result of any cryonics-related procedure including return of spontaneous heartbeat, evidence of respiratory effort (of any kind), responsiveness, or evidence of spontaneous movement?
Per b) above, it should be understood that the first criterion to be satisfied when pronouncing death in all published procedures, protocols and articles which I have been able to find that instruct physicians and other medical, paramedical and law enforcement personnel in how to pronounce death is not determining the absence of respiration and circulation, but rather establishing the absence of any evidence of responsiveness or spontaneous movement of any kind. Simply put, the first injunction given the person who would pronounce death is to establish that there are no signs of life. The 1980 report Defining Death: A Report on the Medical, Legal and Ethical Issues in the Determination of Death prepared by the President’s Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research states that the following criteria must be met in pronouncing death by clinical (cardiopulmonary) criteria and proposes the following procedural standards in Appendix F on how to pronounce death (32):
“The Criteria for Determination of Death
An individual presenting the findings in either section A (cardiopulmonary) or section B (neurologic) is dead. In either section, a diagnosis of death requires that both cessation of functions, as set forth in subsection 1, and irreversibility, as set forth in subsection 2, be demonstrated.
A. AN INDIVIDUAL WITH IRREVERSIBLE CESSATION OF CIRCULA TORY AND RESPIRATORY FUNCTIONS IS DEAD.
1. CESSATION IS RECOGNIZED BY AN APPROPRIATE CLINICAL EXAMINATION.
Clinical examination will disclose at least the absence of responsiveness, heartbeat, and respiratory effort. Medical circumstances may require the use of confirmatory tests, such as an ECG.
2. IRREVERSIBILITY IS RECOGNIZED BY PERSISTENT CESSATION OF FUNCTIONS DURING AN APPROPRIATE PERIOD OF OBSERVATION AND/OR TRIAL OF THERAPY.
In clinical situations where death is expected, where the course has been gradual, and where irregular agonal respiration or heartbeat finally ceases, the period of observation following the cessation may be only the few minutes required to complete the examination. Similarly, if resuscitation is not undertaken and ventricular fibrillation and standstill develop in a monitored patient, the required period of observation thereafter may be as short as a few minutes.
When a possible death is unobserved, unexpected, or sudden, the examination may need to be more detailed and repeated over a longer period, while appropriate resuscitative effort is maintained as a test of cardiovascular responsiveness. Diagnosis in individuals who are first observed with rigor mortis or putrefaction may require only the observation period necessary to establish that fact.” (Emphasis, underlined text, is mine.)
It is vitally important that the words “an appropriate clinical examination” be understood to be deliberately vague, and to rely on that which constitutes the physician’s “ordinary standards of medical practice” or “according to usual and customary standards of medical practice” or “in accordance with reasonable medical standards” or “in accordance with accepted medical standards”… These statements, which all invoke the synonyms “customary,” ordinary,” “acceptable,” or “reasonable,” are taken from the diverse statutes enacted by the states governing the pronouncement of death (32). This statutory language, as well as the “appropriate clinical examination” language used in the President’s Commission Guidelines is designed to recognize that (quoting the Commission’s report):
“Theoretically, even destruction of an organ does not prevent its functions from being restored. Any decision to recognize “the end” is inevitably restricted by the limits of available medical knowledge and techniques. Since “irreversibility” adjusts to the times, the proposed statute can incorporate new clinical capabilities. Many patients declared dead fifty years ago because of heart failure would have not experienced an “irreversible cessation of circulatory and respiratory functions” in the hands of a modern hospital (32).” (Emphasis theirs.)
The implication of all this “normalizing” language is that any procedures or clinical criteria employed in pronouncing death inherently acknowledge that the case at hand in fact be customary, ordinary, and within the reasonable frame of reference in which the physician commonly, routinely, ordinarily…pronounces death. Both the President’s Commission and the states explicitly recognize that when death is, how it is determined, and what constitutes irreversible are all moving targets and that the physician as an individual, and the medical community as a whole, are charged with responsibility in tailoring the specific diagnostic procedures they apply to the particulars of each case (i.e., the duration of post arrest waiting time, use of ECG to verify cardiac arrest, continued resuscitation efforts in hypothermic patients). To quote the Commission’s report yet again:
“A statute (sic, defining death) should apply uniformly at any one time, but it need not fix at the current level of scientific sophistication or biomedical technology the means by which it is to be implemented. In the terms used earlier, a statute should be confined to the standards by which death is to be determined and leave to experts in biomedicine the continuing development of criteria and specific tests that fulfill them (32).”
Restoration of any signs of life due to application of cryonics procedures, by definition, defeats the universal requirement of irreversibility or permanence which is inherent in all legally, medically and socially accepted definitions and criteria for determining and pronouncing death – from the Common Law definition as defined in Black’s Law Dictionary (33) to the commonsense definition as defined in Webster’s (34). The criterion that the “permanence” or “irreversibility” of the loss vital signs obtain is also called for in the Harvard Criteria (34), the American Medical Association’s guidelines (35), the landmark Kansas statue defining death (36) and the Uniform Declaration of Death Act (37)†.
Figure 5: The Premature Burial painted by Dutch artist Antoine Wiertz is as evocative today of the discomfort and anxiety felt by much of humanity when contemplating the prospect of ambiguity or error in determining when death occurs (and being certain of its permanence) as it was when Wiertz painted it in 1854.
What this means is that the decision to provide cardiopulmonary support at any time after the patient’s medico-legal death has been pronounced must, at a minimum, satisfy the criterion of irreversibility by not restoring any spontaneous signs of life including movement, agonal gasping, agonal respiration, return of mechanical or electrical activity in the heart (ECG), or return of electrical activity in the brain (EEG). Absent pharmacological intervention, it is inevitable that one, or even all of these signs, including consciousness and responsiveness to verbal stimuli, will return in a significant population of cryopatients subjected to prompt cardiopulmonary support.
While a waiting period of 5 or 10 minutes after cardiac arrest has been proposed as sufficient to prevent the return of cerebral function under normal clinical conditions (39), this is by no means assured, and in many patients mild hypothermia and compensatory metabolic changes associated with pre-mortem pathologies that cause chronic ischemia or hypoxia (such as congestive heart failure or chronic obstructive pulmonary disease) or a prolonged agonal period, may extend the window of cerebral recoverability well beyond this interval. Additionally, on no account will such a short waiting period, or even a waiting period as long as 20 minutes, insure that there is not a return of spontaneous cardiac activity (40), agonal gasping, or reflexive movements in response to chest compressions or other manipulations which stimulate the spinal cord (41), (42), Indeed, agonal gasping has been documented in one study to occur in 46% of arrests secondary to myocardial infarction or other primary cardiac causes, and in 32% of arrests from other etiologies (43), (44). It is also important to note that there appears to be a “plateau effect” where there is less than one-third variability in survival with intact to moderate neurological disability between moderate (5-15 min) and prolonged (>15 min) periods of cardiac arrest (45), (7) (46),. The best estimate of the upper limit of survival in cardiac arrest in the pre-hospital setting is based upon the observation that there are no survivors of normothermic arrest beyond an interval of 30 minutes from the time of witnessed collapse to initiation of basic cardiac life support (BCLS); although survival does occur in a few cases where the interval between arrest and BCLS is estimated to have been as long as 30 minutes (47), (45).
PEA Reconsidered
In many patients dying slowly the cessation mechanical contraction of the heart is followed by an interval of continued electrocardiographic activity; pulseless electrical activity (PEA), formerly known as “electromechanical disassociation” (EMD). The likely frequency of PEA in the population of cryopatients who experience slow deaths is the reason why ECG is never used as a monitoring or validating modality for determining or pronouncing medico-legal death (since some clinicians and nurses are unwilling to pronounce if PEA is present). The fact that PEA was likely to return in a significant fraction of patients undergoing CPR was deemed irrelevant since survival following PEA was considered virtually non-existent. Thus, in unmonitored cryopatients, PEA was considered simply an undesirable artifact of cardiopulmonary support which, especially if undetected (i.e., no ECG monitoring in place), was irrelevant. Indeed, in many hospitals in the U.S. terminal patients exhibiting PEA are still disconnected from the ECG monitor and then pronounced using clinical criteria.
__________________________________________________________________
Understanding PEA in a Cryonics Context
PEA occurs when cardiac contractions are absent in the presence of coordinated electrical activity. The electrocardiogram (ECG) may look virtually normal, as shown A above, or it may reflect a global insult to the myocardium with a slow and/or widened QRS-complex bradycardia as seen in the ECG from a patient who arrested after a long period of hypoxia secondary to lung cancer in B, above. This rhythm is typical of global myocardial energy depletion secondary to hypoxia, acidosis, hyperkalemia, and ischemia.
PEA is caused by the inability of the myocardium to generate sufficient force to cause mechanical contraction despite electrical depolarization. The electromechanical decoupling seen in PEA can occur as a result of a wide array of pathologies with hypoxia secondary to respiratory failure, hypotension due to hypovolemia (dehydration, sepsis hemorrhage) being the most common causes. The underlying physiological mechanisms are:
• Decreased preload: Cardiac sarcomeres require an optimal length prior to contraction (i.e., preload). If this length is not available because of volume loss or pulmonary embolus (causing decreased venous return to the left atrium), the left ventricle is unable to generate sufficient pressure to contract. Cardiac tamponade also may cause decreased ventricular filling.
• Decreased contractility: Optimal myocardial contractility is determined by optimal filling pressure, afterload, and the presence and availability of inotropic substances (e.g., epinephrine, norepinephrine, digoxin, calcium). Calcium influx and binding to troponin C is essential for cardiac contraction. If calcium is not available (e.g., with calcium channel blocker overdose) or if calcium’s affinity to troponin C is decreased (as in hypoxia), contractility suffers. Depletion of intracellular ATP reserves causes an increase in ADP, which can bind calcium, further reducing energy reserves. Excess intracellular calcium can result in reperfusion injury by causing severe damage to the intracellular structures, predominantly the mitochondria.
Afterload is inversely related to cardiac output. Severe increases in afterload, as often occurs in decompensated congestive heart failure, cause a decrease in cardiac output. However, increased afterload alone is rarely the cause of PEA. The causes of PEA in the cryopatient (in order of likelihood) are: Hypoxia, Hypovolemia, Hyperkalemia, Myocardial infarction, Pulmonary Embolism, Hypoglycemia, Hypokalemia, Cardiac Tamponade, and very rarely Tension Pneumothorax or Drug Intoxication (overdose).
__________________________________________________________________
PEA is common in slowly dying cryopatients (~60%) because the final common pathway in such arrests is typically hypoxia secondary to hypovolemia, space occupying lesions of the lungs (cancer, COPD), pulmonary edema in the setting of multiple system organ failure (MSOF) or circulatory collapse with respiratory arrest as a result of sepsis or hemorrhage. To understand the likely incidence of PEA in cryopatients it is useful to consider that the incidence of PEA in monitored patients dying in hospital was 68% in one study (3) while most studies report the incidence between 30-40% of all in-hospital deaths (4), (7), (8). Yet another reason why PEA is likely to occur with greater frequency in the slowly dying cryopatient is that many such patients are hypercoagulable and, if this not treated (as is so often the case) arrest may occur as a result of pulmonary embolism, another significant cause of PEA.
However, the medical perception, as well as the medical reality, of the incidence and prognosis of survival in cases of PEA in patients presenting with sudden cardiac death (SCD), as well as in patients suffering from other causes of cardiac arrest is undergoing a sea-change. In the past the PEA was exceedingly rare and its presence in either in-hospital or out-of-hospital cardiac arrest patients was considered a “hopeless” cardiac rhythm that few if any patient’s survived (48). For reasons not yet fully understood PEA has gone from being a rare presenting rhythm in cardiac arrest to the most common presenting rhythm in both in-hospital (49), (49), (8) and out-of-hospital cardiac arrests (49), (50). While the prognosis for survival of patients with PEA is still poor, it is by no means hopeless and appears to be steadily improving (48). The likely return of PEA during CPS in cryopatients may thus take on added medico-legal significance and the return of PEA, ventricular fibrillation, or other non-perfusing rhythms in cryopatients with implanted automatic defibrillators (increasingly likely as indications for use and application of these devices rapidly expands) would result in these devices administering countershocks with accompanying visible movement of the patient.
Damned If You Do and Damned If You Don’t?
If CPS is to be undertaken at any reasonable time interval after cardiopulmonary arrest and pronouncement (i.e., < 1 hour post arrest) without the attendant risks of the return of cardiac and cerebral electrical activity, as well as the more visible and disturbing risks of the return of spontaneous movement, agonal gasping, agonal respirations, or the return of spontaneous circulation, it will be necessary to intervene pharmacologically. It then becomes a question of not whether pharmaco-prevention of life signs should be done, but rather how it should be done. Further, I believe that when pharmaco-prevention is undertaken there must be no dissembling or secrecy. I know of no rational argument why it should be undertaken with anything but complete transparency; secrecy in such a matter is neither sustainable nor desirable.
The ethics of administering compounds which prevent the return of any vital signs, including electrophysiological ones (EEG and ECG) in a patient who has been pronounced dead by a disinterested physician using “accepted, customary, ordinary or reasonable” medical and legal standards may be debatable, however the legality of the procedure is not; it is not possible to kill a dead man and the law of double effect does not apply to a cadaver. The occurrence of movement in a cryopatient, or other signs unequivocally associated life are inevitable and will, with equal inevitability, eventually be witnessed by non-cryonicist stabilization staff, as well by family, other bystanders, and any medical or paramedical personnel who happen to be present and watchful when the event occurs. The medical, legal, ethical and public relations repercussions from such an event are not difficult to imagine. Even if no change in the law occurs as a result, the public relations effects of such an incident could well have the same practical effect as an outright ban on cryonics or cryonics stabilization operations. Hospitals, hospices, extended care facilities, mortuaries, and other institutions whose cooperation is essential to the delivery of cryonics services might refuse to deal with cryonics organizations, and conceivably even with individuals who wish to be cryopreserved.
The British Catastrophe?
Many in the cryonics community seem to regard the likelihood of a medico-legal ban on cryonics stabilization procedures as something abstract, remote, and not likely to occur in the absence of some provoking event. For cryonicists living in Britain (and arguably all of the United Kingdom) prohibition of the application of any kind of circulatory support to patients pronounced dead by clinical criteria appears close to being a reality if it has not already occurred. In April of 2006 a Working Party established through the Royal College of Anaesthetists on behalf of the Academy of Medical Royal Colleges and the English Department of Health presented a draft of “A Code of Practice for the Diagnosis and Certification of Death” which substantially revises the 1998 “Code of Practice for the Diagnosis of Brain Stem Death.”
A major reason this revision was undertaken was to prevent the immediate post-pronouncement use of non-beating heart donors (NBHD) in organ transplantation. NBHD is highly controversial in much of the western world since it typically involves rapid post mortem interventions to protect the donor’s organs from ischemic injury including the application of CPR (51) and often the use of cardiopulmonary bypass to maintain organ viability (39), (52), (53). The use of immediately applied post-pronouncement preservation techniques has become routine in the Netherlands and organs from NBHD donors now constitutes 40% of kidneys transplanted there (54). The revised British code of practice expressly forbids application of any kind of cardiopulmonary support (both CPR and CPB) to patients pronounced dead on the basis of clinical criteria (as opposed to those pronounced dead by neurological or so-called “brain death” criteria. Discussion on the draft document was closed on 18 August, 2006 (55) and the code was scheduled to be adopted before January of 2007†. The last paragraph of the revised code under the subheading “Certifying Death After Cardiorespiratory Arrest” clearly states:
“It is obviously inappropriate to initiate any intervention that has the potential to restore coronary or cerebral perfusion, including chest compressions or the institution of cardiopulmonary bypass after death has been certified.”
This document also, for the first time, establishes a prescribed evaluation (waiting) period for determining cardiorespiratory arrest, namely 5 minutes. This development demonstrates clearly that events in biomedicine far removed from the concerns of cryonicists can have profound negative impact – not all biomedical advances promise beneficence. Here in the U.S. the debate over NBHD has become intense and often bitter (56), (57), (58),. It seems well within the realm of possibility that the actions of some transplant surgeons and patient advocacy groups who are pushing the envelope to expand NBHD may result in a similar revision to U.S. law (59), (60).
Novel Pharmacological Approaches
While concern over the adverse reputation of drugs such as potassium chloride and pancuronium bromide may be justified, it is not acceptable to eliminate them from the stabilization protocol and simply hope that the problems that they were originally included to address will go away. If these drugs are deemed to be too much of a perceived medico-legal liability, then alternative agents must be identified and validated. The now classic work of Susan Gower Smith established that reversible (survivable) paralysis of the voluntary muscles can be achieved with intravenous administration of magnesium sulfate in the dog at a dose of 0.25 g/kg with a dose ~0.30 g/kg resulting in complete paralysis of both the respiratory and skeletal musculature (61). This work also established the antagonism of potassium to magnesium-induced paralysis, underscoring the fact that if the magnesium ion is substituted for pancuronium or other traditional (neuromuscular blocking) paralytic drugs, the potassium ion cannot be used to secure cardioplegia and electrocardio and electrocerebral silence. While the dose of magnesium sulfate required to secure complete paralysis of the voluntary muscles is a staggering 22.5 grams for a 75 kg man, it is not unsupportable if other adjustments to reduce the total number of osmoles given during stabilization are made, such as eliminating the administration of 20% mannitol. Unfortunately, the use of such a large (and hyperosmotic) dose of magnesium sulfate might preclude the potentially very promising use of hypertonic saline as a valuable neuroprotective and microcirculation enhancing drug in cryopatient stabilizations (62).
If the potassium ion is deemed acceptable absent pancuronium bromide, it will act as a paralytic at the same dose at which it was previously used to ensure cardioplegia and electrocerebral silence (30 mEq/kg); this is based on clinical experiences where hyperkalemic paralysis has preceded cardiac arrest (62), (63),(64), (65). If potassium is not deemed acceptable, then non-depolarizing cardioplegia employing a whole blood concentration of 200 micromol/L adenosine and 500 micromol/L lidocaine can be used to prevent the return of both mechanical and electrical activity in the heart (66).
A much more difficult problem is achieving electrocerebral silence with an extant, approved (ethical) injectable medication without recourse to barbiturates (virtually impossible because their scheduled status) or doses of propofol that would result in unacceptable hypotension. Several alternative approaches suggest themselves, including the use of the inexpensive inhalation anesthetic isoflurane at high mean alveolar concentrations as a substitute for propofol, and the use of combinations of metabolic inhibitors such as hydrogen sulfide or hydrogen sulfide donors (67), (68), (69), (69), carbon monoxide or other heme oxygenase-1 inducers and/or p38 mitogen activated protein kinase modulators (70), (71), (72), (73), 5’-adenosine monophospohate (74), and the inactive anomer of NADH; α –NADH (75). Metabolic inhibitors and hibernation/hypothermia mimetic molecules (so-called “suspended animation-inducing drugs”) are particularly attractive to suppress EEG activity because of their profound cytoprotective effects in both normothermic and cold ischemia (i.e., organ preservation) (76),(77),(78).
All of the approaches discussed in the preceding paragraph will require validation using translational research in an appropriate animal model. Hydrogen sulfide, while certainly capable of inhibiting metabolism and inducing torpor in mice has not been demonstrated to have similar effects in sheep, raising questions about its efficacy in large mammals (79). Hydrogen sulfide also has complex and contradictory effects; it can provide systemic and myocardial protection against hypoxia and ischemia, but exacerbates neuroinjury in a model of stroke; probably by up-regulating NMDA receptor function through activation of adenyl cyclase (80). While adenosine has broad cytoprotective properties and can assist in inducing torpor, it induces profound and sustained hypotension at doses far below those required to achieve non-depolarizing cardioplegia (81). It seems likely that these first generation metabolism-moderating molecules will of service primarily in elucidating the biochemical mechanics of torpor and that practical application in the near term will require considerable finesse and a great deal of combinatorial research. It seems equally likely that more targeted species will emerge over the course of the next 2-3 years.
Phenytoin, an anticonvulsant with structural similarity to the barbiturates, has been proposed as a substitute for potassium chloride in preventing the return of ECG and EEG in cryopatients (82). Phenytoin acts by blocking voltage-dependent sodium channels, limiting the propagation of seizure discharge (83). This response is mediated by a use-dependent and voltage-dependent slowing in the rate of recovery of voltage-activated sodium channels from inactivation (84). When given rapidly by the intravenous route, a high dose of phenytoin causes cardiac arrest by inducing ventricular arrhythmias due to acute, massive blockade of the sodium channels (85). Such rapidly IV administered high doses of phenytoin also results in profound, refractory hypotension due to systemic vasodilatation; both arterial and venous (83). Comparable oral doses of the drug do not typically cause these effects (86). Numerous reviews of phenytoin intoxication and poisoning document coma, often with seizures, but give no indication that phenytoin is effective at securing electrocerebral silence or in suppressing the ECG or EEG (87), (88), (85), (89). The lethal effects of rapidly IV administered phenytoin are likely to be transient in the setting of extended artificial circulation and ventilation since they appear due to the rapidity of sodium channel blockade and do not seem to be dependent upon the absolute concentration of the drug (90). Indeed, there is speculation that the arrythmygenic effects of rapidly administered IV phenytoin may be due to the vehicle used to administer the drug (propylene glycol) (91) since such effects are rare with the water soluble analog of phenytoin, phosphenytoin (92). In any event, the profound vasodilatation and hypotension associated with rapid, high dose IV phenytoin administration would seem to preclude its use as a medication in cryopatient stabilization.
Conclusion
Cryonicists face the difficult choice of either abandoning cardiopulmonary support during stabilization operations, returning to the use of the previously employed drugs to ensure cardiocerebral arrest and complete skeletal muscle paralysis, or adopting novel pharmacological strategies to achieve these ends. The current position of ignoring the problem and awaiting the inevitable publicly witnessed return of motor activity, agonal gasping, agonal respirations and/or spontaneous cardiac activity in a cryopatient undergoing CPS is unacceptable. It is the responsibility of all cryonics organizations using CPS to rapidly implement both interim and long-term solutions to this problem.
All cryonics organizations, regardless of the protocols they employ, have a huge stake in the responsible management of this problem. Any truly effective long-term solution will necessarily transcend pharmacology, because the problem is as much social and legislative, as it is biological (38). Cryonics organizations need to work together in a coherent and determined way to make statutory changes in the laws governing pronouncement of death and disposition of anatomical gifts. Changes that specifically recognize and enable the biomedical procedures essential to delivering the highest quality cryonics care. Absent such changes, the law will continue to follow the moving target of irreversibility as it applies to the determination of death until there is an unhappy intersection between our definition of dead and their definition of dead.
REFERENCES:
1. deWolf A. Telephonic discussion regarding elimination of paralytic and cardioplegic from cryonics stabilization protocol. In; 2005.
2. Harris SB. Conversation between the author and Steven B. Harris, M.D. at the 7th Alcor Conference, Hilton Scottsdale Resort. In: Darwin M, ed. Scottsdale, AZ; 2007.
3. Raizes G, Wagner, GS, Hackel, DB: Jan. Instantaneous nonarrhythmic cardiac death in acute myocardial infarction. Am J Cardiol 1977;39(1):1-6.
4. Nadkarni V, Larkin, GL, Peberdy, MA, Carey, SM, Kaye, W, Mancini, ME, Nichol, G, Lane-Truitt, T, Potts, J, Ornato, JP, Berg, RA. First documented rhythm and clinical outcome from in-hospital cardiac arrest among children and adults. JAMA 2006;4(295):50-7.
5. Confidential Communication with Suspended Animation, Inc. staff member. In; 2005.
6. Confidential Communication with Alcor Life Extension Foundation, Inc., consultant. In; 2002.
7. van Walraven C, Forster, AJ, Stiell, IG. Derivation of a clinical decision rule for the discontinuation of in-hospital cardiac arrest resuscitations. Arch Intern Med 1999;159:129-34.
8. Cooper S, Cade, J. Predicting survival, in-hospital cardiac arrests: resuscitation survival variables and training effectiveness. Resuscitation 1997;35:17-22.
9. Sullivan M. Personal Communication. In: Darwin M, ed.; 2007:Discussion on forensic impact of cryopatient stabilization medications.
10. Human Cryopreservation Stabilization Medications. Alcor Life Extension Foundation, Inc., 2007. (Accessed September 9, 2007, at http://www.alcor.org/Library/html/stabilizationmeds.html.)
11. Wysowski D, Pollock, ML. Reports of death with use of propofol (Diprivan) for nonprocedural (long-term) sedation and literature review. Anesthesiology 2006;105:1047-51.
12. Wasek S. Dueling over propofol. Outpatient Surg Mag 2005;5(10):32-7.
13. Flynn G. “Poachers and dabblers?” ASA president’s incautious comment riles emergency physicians. Ann Emerg Med 2007;50(3):264-7.
14. Propofol sedation: Who should administer? Institute for Safe Medication Practices, 2005. (Accessed September 9, 2007, at http://www.ismp.org/.)
15. Veterinary Euthanasia Procedures: Survey Results (Nov 11, 2002 thru Dec 28, 2002). Veterinary Information Network, Inc., 2002. (Accessed September 9, 2007, at http://test.vin.com/Survey_System/test.plx?type=2&which=EUTHANASIA_PROCEDURES&ID=ok&action=review.)
16. Cornick-Seahorn JL. Veterinary Anesthesia: Butterworth-Heinemann; 2000.
17. Kormer G, inventor; Injectable propofol formulations. United States patent 5,962,536.
1999.
18. AstraZeneca. Diprivan (propofol) Injectable Emulsion. In. 30193-00 Rev 08/05 ed. Caponago, Italy: AstraZeneca Pharmaceuticals LP; 2005.
19. Branson K, Gross, MR. Propofol in veterinary medicine. Journal of the American Veterinary Medical Association 1994;204(12):1888-90.
20. Baudoin Z. General anaesthetics and anaesthetic gases. Amsterdam: Elsevier.
21. Yorker B, Kizer, PW, Lampe, P, Forrest, ARm, Lannan, JM, Russell, DA. Serial Murder by Healthcare Professionals. Journal of Forensic Sciences
2006;51(6):1362-71.
22. Kinnell H. Serial homicide by doctors: Shipman in perspective. BMJ 2000;321:1594-7.
23. Darwin M, Harris, SB, Russell, SR, O’Farrell, Rasch, C, J, Pengelle, C, Fletcher, M. Routine Resuscitation of Dogs from 15-17 Minutes of Normothermic Ischemia (37.5°C) With Long Term Survival (>6 weeks). In: 21st Century Medicine Seminar on Recent Breakthroughs in Cryobiology and Resuscitation Research. Ontario, CA; 1998.
24. Hahn S, Sullivan, FJ, DeLuca, AM, Bacher, JD, Liebmann, J, Krishna, MC, Coffin, D, Mitchell, JB. Hemodynamic effect of the nitroxide superoxide dismutase mimics. Free Radic Biol Med 1999;27((5-6)):529-35.
25. Darwin M. Transport Protocol for Cryonic Suspension of Humans, Fourth Edition. 1990.
26. Best B. Telephonic communication regarding the prohibition on photograhy and videography during human cryopreservations at the Cryonics Institute. 2006.
27. Platt C. Conversation about prohibition of photography and videography of Alcor human cryopreservation cases. In. Boynton Beach, FL; 2006.
28. Toshiba EVR Series Security DVR With 4 Terabytes of Memory. Toshiba America Information Systems, Inc., 2006. (Accessed at http://www.mp50.com/8070/DVRUPG1RT525TR5.asp.)
29. Castro H. Police cars get digital cameras; Seattle department first to use new wireless capability. In: Seattle Post-Intelligencer Reporter; 2004.
30. Digital video recorders give more reliable, accurate footage to police. The Enquirer. (Accessed September 8, 2007, at http://www.policeone.com/police-products/vehicle-equipment/in-car-video/articles/99438/.)
31. Cylon Body Worn Surveillance System. Audax Group, 2007. (Accessed September 9, 2007, at http://www.intelcam.co.uk/.)
32. Defining Death: A Report on the Medical, Legal and Ethical Issues in the Determination of Death prepared by the President’s Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research. In. Washington, D.C.: Government Printing Office; 1981.
33. Garner BA. Black’s Law Dictionary: Thompson West; 2004.
34. Webster’s Revised Unabridged Dictionary. Springfield: G & C. Merriam Co.; 1913.
35. AMA. Guidelines for the determination of death. JAMA 1981;246(19):2184-6.
36. Capron A, Kass, LR. A statutory definition of the standards for determining human death (Kans Stat Ann (suppl 197 1):77-202.). Univ Pa L Rev 1978:87-118.
37. Uniform Determination of Death Act. Chicago: National Conference of Commissioners on Uniform State Laws; 1981 February 10.
38. Lizza JP. Persons, Humanity, and the Definition of Death. Boston: Johns Hopkins University Press; 2006.
39. DeVita M, Snyder, JV., Jun. Development of the University of Pittsburgh Medical Center policy for the care of terminally ill patients who may become organ donors after death following the removal of life support. Kennedy Inst Ethics J 1993;3(2):31-43.
40. Vukmir R, Bircher, N, Radovsky, A, Safar, P. Sodium bicarbonate may improve outcome in dogs with brief or prolonged cardiac arrest. Crit Care Med 1995;23:515-22.
41. Jain S, DeGeorgia, M. Brain death-associated reflexes and automatisms. Neurocrit Care 2005;3(2):122-6.
42. Dosemeci L, Cengiz. M, Yilmaz, M, Ramazanoglu, A. Frequency of spinal reflex movements in brain-dead patients. 2004;36(1):17-9.
43. Clark J, Larsen, MP, Culley, LL, Graves, JR, Eisenberg, MS. Incidence of agonal respirations in sudden cardiac arrest. Ann Emerg Med 1992;21(12):1464-7.
44. Rea TD. Agonal respirations during cardiac arrest. Curr Opin Crit Care 2005;11(3):188-91.
45. Vukmir R. Survival from prehospital cardiac arrest is critically dependent upon response time. Resuscitation 2006;69(2):229-34.
46. Herlitz J, Svensson, L, Engdahl, J, ¨Angquist, K. Silfverstolpe, J, Holmberg, S. Association between interval between call for ambulance and return of spontaneous circulation and survival in out-of-hospital cardiac arrest. Resuscitation 2006;71:40-6.
47. DeBehnke D. Resuscitation time limits in experimental pulseless electrical activity cardiac arrest using cardiopulmonary bypass. Resuscitation 1994;27(3):221-9.
48. Parish D, Dinesh, KM, Francis, C, Dane, C. Success changes the problem: Why ventricular fibrillation is declining,why pulseless electrical activity is emerging, and what to do about it. Resuscitation 2003;58:31-5.
49. Parish D, Dane, FC, Montgomery, M, Wynn, LJ, Durham, MD, Brown, TD. Resuscitation in the hospital: relationship of year and rhythm to outcome. Resuscitation 2000;47:219-29.
50. Stiell I, Wells, GA, Field, BJ, et al. Improved out-of-hospital cardiac arrest survival through the inexpensive optimization of an existing defibrillation program. JAMA 1999;281:1175-81.
51. Quintela J, Gala, B, Baamonde, I, Fernandez, C, Aguirrezabalaga, J, Otero, A, Suarez, F, Fernandez, A, Gomez, M. Long-term results for liver transplantation from non-heart-beating donors maintained with chest and abdominal compression-decompression. Transplant Proc 2005;37(9):3857-8.
52. Fukushima N, Shirakura, R, Chang, JC, Izutani, H, Inoue, M, Yamaguch,i T, Kobayashi, Y, Yoshitatsu, M, Ahamet, I, Saito, S, Matsuda, H. Successful experimental multiorgan transplant from non-heart-beating donors using percutaneous cardiopulmonary support. ASAIO J 1998;44(5):M525-8.
53. Koyama I, Shinozuka, N, Miyazawa, M, Watanabe, T. Total body cooling using cardiopulmonary bypass for procurement from non-heart-beating donors. Transplant Proc 2003;34(7):2602-3.
54. Daemen J, de Wit, RJ, Bronkhorst, MW, Yin, M, Heineman, E, Kootstra, G. Non-heart-beating donor program contributes 40% of kidneys for transplantation. Transplant Proc 1996;28(1):105-6.
55. Simpson P. Letter from Dr. Peter Simpson, Working Party Chairman President, Royal College of Anaesthetists soliciting comments on the Revised Code of Practice for the Diagnosis and Certification of Death in Britain. In; 2007.
56. Fox R. “An ignoble form of cannibalism”: reflections on the Pittsburgh protocol for procuring organs from non-heart-beating cadavers. Kennedy Inst Ethics J 1993;3(2):231-9.
57. Doig C, Rocker, G. Retrieving organs from non-heart-beating organ donors: a review of medical and ethical issues. Can J Anaesth 2003;50(10):1069-76.
58. Bos M, 1 M. Ethical and legal issues in non-heart-beating organ donation. Transplantation 2005;5;79(9):1143-7.
59. Cole D. Statutory definitions of death and the management of terminally ill patients who may become organ donors after death. Kennedy Inst Ethics J 1993;3(2):145-55.
60. Brook N, Waller, JR, Nicholson, ML. Nonheart-beating kidney donation: current practice and future developments. Kidney Int 2003;63(4):516-29.
61. Smith S. Respiration and Paralysis as They Relate to Magnesium-Potassium Antagonism. Am J Physiol Mar; 1951;164(3):702-9.
62. Fluid Resuscitation: State of the Science for Treating Combat Casualties and Civilian Injuries. Washington, DC: Institute of Medicine and National Academy Press; 1999.
63. Richardson G, Sibley, JC. Flaccid quadriplegia associated with hyperpotassaemia. Can Med Assoc J 1953;69:504-6.
64. Udezue E, Harrold, BP. Hyperkalaemic paralysis due to spironolactone. Postgrad Med J 1980;56:254-45.
65. Freeman S, Fale, AD. Muscular paralysis and ventilatory failure caused by hyperkalemia. Br J Anaesth 1993;70:226-7.
66. Dobson G, Jones, MW. Adenosine and lidocaine: a new concept in nondepolarizing surgical myocardial arrest, protection, and preservation. J Thorac Cardiovasc Surg 2004;127(3):794-805.
67. Blackstone E, Roth, MB. Suspended animation-like state protects mice from lethal hypoxia. Shock 2007;27(4):370-2.
68. Lowicka E, Beltowski, J. Hydrogen sulfide (H2S) – the third gas of interest for pharmacologists. Pharmacol Rep 2007;59(1):4-24.
69. Pan T, Feng, ZN, Lee, SW, Moore, PK, Bian, JS. Endogenous hydrogen sulfide contributes to the cardioprotection by metabolic inhibition preconditioning in the rat ventricular myocytes. J Mol Cell Cardiol 2006;40(1):119-30.
70. Vera T, Henegar, JR, Drummond, HA, Rimoldi, JM, Stec, DE. Protective effect of carbon monoxide-releasing compounds in ischemia-induced acute renal failure. J Am Soc Nephrol 2005;6.(4):950-8.
71. Ryter S, Alam, J, Choi, AM. Heme oxygenase-1/carbon monoxide: from basic science to therapeutic applications. Physiol Rev 2006;86(2):583-650.
72. Hoetzel A, Schmidt, R. Kohlenmonoxid –Gift oder potenzielles Therapeutikum? Anaesthesist 2006;55:1068-79.
73. Amersi F, Shen, XD, Anselmo, D, Melinek,J, Iyer, S, Southard, DJ, Katori, M, Volk.HD, Busuttil, RW, Buelow, R, Kupiec-Weglinski, JW. Ex vivo exposure to carbon monoxide prevents hepatic ischemia/reperfusion injury through p38 MAP kinase pathway. Hepatology 2002;5(4):815-23.
74. Lee CC, inventor; THE BOARD OF REGENTS OF THE UNIVERSITY OF TEXAS SYSTEM, assignee. METHODS AND COMPOSITIONS FOR INDUCING TORPOR IN A SUBJECT. United States. 2007 September 13, 200.
75. Anderson T, Li, CQ, Shao, ZH, Hoang, T, Chan, KC, Hamann, KJ, Becker, LB, Vanden Hoek TL. Transient and partial mitochondrial inhibition for the treatment of postresuscitation injury: getting it just right. Crit Care Med 2006;34((12 Suppl)):S474-82.
76. Fang X, Tang, W, Sun, S, Weil, MH., Dec. delta-Opioid-induced pharmacologic myocardial hibernation during cardiopulmonary resuscitation. Crit Care Med 2006;34(12 Suppl):S486-9.
77. Schwartz C, Georges, AJ, Gallagher, MA, Yu, L, Kilgore, KS, Bolling, SF. Delta opioid receptors and low temperature myocardial protection. Ann Thorac Surg 1999;68(6):2089-92.
78. Borlongan C, Wang, Y, Su, TP. Delta opioid peptide (D-Ala 2, D-Leu 5) enkephalin: linking hibernation and neuroprotection. Front Biosc 2004;9:3392-8.
79. Blackstone E, Morrison, M, Roth, M. H2S Induces a Suspended Animation-Like State in Mice. Science 2005;308(5721): 518.
80. Qu K, Chen, PLHC, Halliwell, B, Moore, PK, Wong, PTH. Hydrogen Sulfide Is a Mediator of Cerebral Ischemic Damage. Stroke 2006;37:889-93.
81. Bulley S, Wittnich, C. Adenosine infusion: a rational approach towards induced hypotension. Can J Cardiol 1995;11(4):327-34.
82. Harris SB. Conversation between the author and Steven B. Harris, M.D. at the 7th Alcor Conference held at the Hilton Scottsdale Resort. In. Scottsdale, AZ; 2007.
83. Hardman J, Limberd, LE, Gilman, AG, eds. Goodman and Gilman’s pharmacological basis of therapeutics. 10th ed. New York: McGraw Hill; 2001.
84. Seger D. Anticonvulsant medications. In: Dart R, Caravati, EM, McGuigan, MA, et al., eds., ed. Medical toxicology. 3rd. ed. Philadelphia: Lippincott Williams & Wilkins; 2004:789–804.
85. Osborn H. Phenytoin and fosphenytoin toxicity. In: Tintinalli J, Kelen, GD, Stapczynski, JS, eds., ed. Emergency medicine: a comprehensive study guide. 6th ed. New York: Mc-Graw Hill; 2004:1117-21.
86. Craig S. Phenytoin Poisoning. Neurocrit Care 2005;3:161–70.
87. Larsen J, Larsen, LS. Clinical features and management of poisoning due to phenytoin. Med Toxicol Adverse Drug Exp 1989;4:229–45.
88. Klasco R, ed. MICROMEDEX Poisindex® Managements: Phenytoin. Greenwood Village, CO.: MICROMEDEX, Thomson.
89. Mellick L, Morgan, JA, Mellick, GA. Presentations of acute phenytoin overdose. Am J Emerg Med 1989;7(1):61-7.
90. DeToledo J, lowe, MR, Rabinstein. A, Villaviza, N. Cardiac arrest
after fast intravenous infusion of phenytoin mistaken for fosphenytoin. Epilepsia 2001;42:288.
91. Golightly L, Smolinske, SS, Bennett, ML, Sutherland, EW 3rd, Rumack, BH. Pharmaceutical excipients. Adverse effects associated with inactive ingredients in drug products (Part I). Med Toxicol Adverse Drug Exp 1988;3(2):128-65.
92. Tiller J, Birkett, D, Burns, R, et al., Guidelines L. Antiepileptics: phenytoin and fosphenytoin. In: Therapeutic guidelines: neurology. North Melbourne, Victoria, Australia: Therapeutic Guidelines, Ltd.; 2002:4-5.
† This is not to imply that propofol is not a safe and effective drug. In fact, the incidence of adverse effects with diprivan is lower than with many other parenteral anesthetics.
† The Uncertainty of the Signs of Death and the Danger of Precipitate Interments, Paris 1740.
‡ An upend example is the Toshiba EVR RAID-5 (redundant backup system) 32 channels DVR 480 fps (15 fps per cam) security video recorder which can accommodate up to 4 terabytes of memory and retails (1 terabyte) for just under $6,000. Such a system would allow continuous video surveillance of every room of a large residence with 6-weeks of audio-video storage capacity.
† Included here is not just the use of drugs, but the use of procedures such the acute induction of hypothermia and the application of any kind of cardiopulmonary support, such as CPR or cardiopulmonary bypass.
† An excellent review of the medico-legal definition of death and the problem presented by the requirement for permanence or irreversibility can be found in Persons, Humanity, and the Definition of Death by John P. Lizza (Lizza JP. Persons, Humanity, and the Definition of Death. Boston: Johns Hopkins University Press; 2006.).
† I have written to Dr. Peter Simpson the Working Party Chairman President to inquire as to the current status of the revised code and to obtain a copy of the most recent draft , or in the event it has been enacted, the final version.